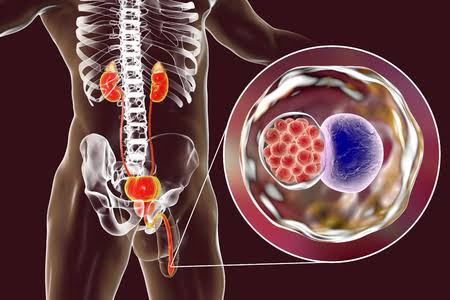
1. “It’s probably just a bladder infection…” – Why chlamydia is easy to overlook
“Going to the bathroom stings a little, and there’s a bit more discharge than usual…
It feels awkward to go to the doctor, so I’ll just wait and see.”
A lot of people think this way and end up letting the problem grow.
But these can actually be early chlamydia symptoms – things like mild itching, unusual discharge, or burning when you pee.
Chlamydia is a sexually transmitted infection (STI) caused by a bacteria called Chlamydia trachomatis.
It’s one of the most common STIs worldwide, and it’s especially frequent in people in their teens, 20s, and early 30s.
The two biggest problems with chlamydia are:
- Symptoms are very mild or completely absent, so many people don’t realize they’re infected.
- When it’s left untreated, it can lead to pelvic inflammatory disease, fallopian tube damage, infertility, and ectopic pregnancy.
While going through the research, one thought kept coming up:
“Most people would definitely brush off these symptoms as something minor.”
So in this post, let’s walk through the essentials in a simple way, and cover everything in one place:
Causes, symptoms, testing, treatment, and prevention of chlamydia.

2. What is chlamydia? A simple breakdown of causes and transmission
2.1 What kind of infection is chlamydia?
Chlamydia is a bacterial sexually transmitted infection.
It can affect the:
- Genitals
- Urethra
- Cervix
- Rectum
- Throat (pharynx)
- Eyes (conjunctiva)
In simple terms, you can think of it as a bacterial infection passed through sexual contact.
2.2 How chlamydia spreads: main transmission routes
The main chlamydia transmission routes include:
- Vaginal sex: penetrative vaginal sex without a condom
- Anal sex: receptive or insertive anal sex without a condom
- Oral sex: mouth-to-genital contact
- During childbirth: a baby can be exposed while passing through the birth canal of an infected mother
Your risk goes up if:
- You have sex without condoms and your partner changes frequently
- You’ve had other STIs in the past
- You’re in your late teens or 20s
In other words, the thought of
“It was just once, I’m sure it’s fine”
combined with unprotected sex is often how chlamydia infection starts.
3. Early chlamydia symptoms in men and women – and the trap of “no symptoms”
3.1 Early chlamydia symptoms in men (chlamydia urethritis)
In men, chlamydia often shows up as urethritis, meaning inflammation of the urethra.
Common male chlamydia symptoms include:
- A burning or stinging sensation when urinating
- Clear or whitish discharge from the tip of the penis that may stain underwear
- Redness, irritation, or an itchy feeling around the urethral opening
- In more severe cases, pain or discomfort in the testicles or epididymis (the tube behind the testicle)
When this happens, many people think:
“It’s just a bladder infection.”
“I’m probably just tired or run down.”
But if you’ve recently had unprotected sex, you really should consider the possibility of early chlamydia symptomsrather than dismissing it.
3.2 Early chlamydia symptoms in women and the link to infertility
Women need to be even more careful.
That’s because many women with chlamydia have no noticeable symptoms at all.
If symptoms do appear, they may look like:
- A noticeable increase in vaginal discharge or a change in odor
- A heavy, uncomfortable feeling in the lower abdomen
- Pain during sex, or light bleeding after sex
- Spotting or irregular bleeding between periods
- Mild burning or discomfort when urinating
The problem is that all of these can easily be mistaken for:
- “Just a yeast infection.”
- “Probably a simple vaginal infection.”
- “Maybe just stress or fatigue.”
But for women, there is a serious concern: the risk of infertility from chlamydia.
If the infection spreads to the uterus and fallopian tubes, it can:
- Narrow or block the fallopian tubes
- Interrupt the normal path of the egg
- Increase the risk of subfertility, infertility, and ectopic pregnancy
This is why female chlamydia and infertility risk are often discussed together.
3.3 Why “no symptoms” does not mean “no problem”: the need for regular screening
For women – especially those under 25 or anyone with multiple sexual partners –
even if you feel completely fine, there’s a strong case for regular chlamydia screening.
- No symptoms does NOT mean no infection.
- It often means the infection is quietly progressing in the background, causing damage without being noticed.
That’s the real danger.

4. What happens if you ignore chlamydia? – Complications like infertility and pelvic inflammatory disease
4.1 Complications in women
If chlamydia is not treated and is left to smolder for a long time, women may face:
- Pelvic inflammatory disease (PID) – infection spreading to the uterus, fallopian tubes, and surrounding structures
- Fallopian tube damage – narrowing or blockage of the tubes
- Resulting subfertility or infertility
- A higher risk of ectopic pregnancy (when a fertilized egg implants in the fallopian tube instead of the uterus)
- Chronic pelvic pain and pain during sex
Recent studies also show that women with a history of chlamydia infection are more likely to develop PID and have tubal problems and fertility issues.
That’s where the phrase “chlamydia increasing infertility risk in women” comes from.
4.2 Complications in men
Men are not completely in the clear either.
Untreated chlamydia can lead to:
- Epididymitis: inflammation in the tube that carries sperm, leading to swollen and painful testicles
- Ongoing testicular pain, swelling, and discomfort
- In some cases, a potential link with reduced sperm count or impaired fertility
So for both men and women, ignoring symptoms with a
“I’m sure it’ll go away on its own”
mindset can come back later as a serious fertility or reproductive health issue.

5. Chlamydia testing – when and how to get checked
5-1. When should you consider getting tested?
You should seriously think about chlamydia testing in situations like these:
- You recently had unprotected sex with a new partner.
- You notice early chlamydia symptoms such as unusual discharge, itching, or burning when you pee.
- A sexual partner tells you they tested positive for an STI or chlamydia.
- You’re planning a pregnancy or are already pregnant.
- You’re under 25 and/or have multiple sexual partners.
Even if you feel completely fine, if you fit these categories,
regular STI and chlamydia screening is a very wise move.
5-2. Testing methods: simple and quick
Common chlamydia testing methods include:
- Urine test
- You provide a sample of your first-catch urine, which is then tested for the bacteria.
- Swab test
- For women: a swab is gently used to collect a sample from the cervix or vagina.
- For men: a urethral swab (although many clinics now rely more on urine tests).
- For anyone with a history of anal or oral sex: rectal or throat swabs may be done.
The tests themselves only take a few minutes,
and results typically come back within a few days, depending on the clinic or lab.
6. Chlamydia treatment and cure – how long does it take to clear?
6.1 A curable STI with proper antibiotic treatment
The good news: chlamydia is usually curable with the right antibiotics.
A healthcare provider will prescribe oral antibiotics based on your situation.
In most cases:
- You take the medication for around a week or so (the exact duration can vary).
- Even if your symptoms improve quickly, it’s important to finish the entire course of antibiotics as prescribed.
During this chlamydia treatment period:
- It’s best to avoid sexual activity, or
- At minimum, follow your provider’s guidance and avoid sex until they say it’s safe again.
You can think of this whole process as your chlamydia cure period.
6.2 Why your partner also needs treatment
Here’s a crucial point that many people overlook:
- If only you get treated and
- Your partner does not get tested or treated,
then as soon as you have sex again,
you may be reinfected.
For this reason, healthcare providers often recommend:
“Your current sexual partner should also be tested and treated.”
This isn’t just “your problem” or “their problem” –
it’s a matter of protecting each other’s health together.
6.3 When follow-up (test-of-cure) is needed
A repeat test may be recommended if:
- Your risk of exposure was high
- Your symptoms were severe
- You weren’t able to follow the treatment exactly as prescribed
In those cases, a follow-up test after treatment helps confirm that the infection is truly gone.

7. Preventing chlamydia: 5 practical tips you can use right away
Chlamydia is not “one and done.”
Even after a full cure, there is a real risk of getting infected again.
That’s why prevention and safer sex habits are so important.
Here are five practical prevention tips you can build into your everyday life:
- Make condoms your default
- Use condoms consistently during vaginal, anal, and oral sex.
- This protects not just against chlamydia, but also other STIs.
- Talk about testing before starting a new sexual relationship
- Saying, “I’ve been tested, and I’d feel better if you got tested too,”
is not an awkward attack – it’s a sign of mutual respect and care.
- Saying, “I’ve been tested, and I’d feel better if you got tested too,”
- Schedule regular STI and chlamydia tests
- Especially if you’re under 25 or have multiple partners,
keep the idea of regular, even yearly chlamydia screening in mind.
- Especially if you’re under 25 or have multiple partners,
- Pause sex during treatment
- While you’re on antibiotics, and until your provider says you’re clear,
taking a break from sex significantly reduces the risk of reinfection and spreading it to others.
- While you’re on antibiotics, and until your provider says you’re clear,
- Use anonymous or low-barrier testing and counseling services if needed
- The word “STI” alone can feel heavy and embarrassing.
- But nowadays, many places offer anonymous testing, telehealth, and discreet services.
- Your health is far more important than the temporary embarrassment you might feel.

8. Key takeaways and final thoughts
Let’s quickly recap the main points:
- Chlamydia is one of the most common bacterial STIs worldwide.
- In both men and women, it can show up as:
- Mild itching, discharge, or burning when you pee, or
- No symptoms at all.
- If left untreated:
- In women, it can cause pelvic inflammatory disease, fallopian tube damage, difficulty conceiving, infertility, and ectopic pregnancy.
- In men, it can lead to epididymitis, testicular pain, and possible effects on fertility.
- The good news is that:
- Chlamydia testing is simple – usually a urine test or swab.
- With the right antibiotic treatment, most cases can be fully cured.
- However, it’s important that both you and your partner are tested and treated, and that follow-up testing is done when needed.
- Long term, the key to staying safe is:
- Consistent condom use
- Regular STI screening
- Open, honest conversations about sexual health
If right now you’re dealing with:
- Unexplained discharge, itching, or burning when you pee, or
- You’ve heard from a partner that they may have an STI,
rather than endlessly scrolling through search results and worrying alone,
consider visiting a nearby OB/GYN, urologist, or sexual health/STI clinic for testing and advice.
With a bit of courage to get tested and treated,
chlamydia is a manageable, treatable infection.
If this post helps you protect your own health –
and maybe also encourages one more person to get checked in time –
then it has done its job.
Medical Disclaimer
This information is intended to help you better understand health-related topics and chlamydia in general.
It does not replace a consultation, diagnosis, or treatment plan from a qualified healthcare professional.
For an accurate assessment of your symptoms or condition, please seek medical evaluation and advice from a licensed provider.








최근댓글